
There are combination therapies of oral medications and these are often prescribed to reduce the burden of several medications which can be difficult for people to take. Some oral therapies can be prescribed in liquid form – if the person with diabetes is having difficulty taking their medications speak to the pharmacist or GP.
Injectable combination medications e.g. Xultophy or Suliqua (combinations of insulin and GLP-1 receptor agonists may be prescribed for some people with diabetes who may be prescribed for some people with diabetes who may need both a GLP1 and insulin therapy. If you are unsure of any medications that are being administered to someone with diabetes that you may be caring for, speak with the pharmacist or GP.
Medications should be given as prescribed and in a timely manner. People living with diabetes may develop side effects or may become intolerant to medications at any time, not just when starting therapies. If you have any concerns speak to your GP or usual health care professional.
- All older adults with diabetes and frailty should have their medications reviewed regularly1Sinclair A (2019) Key learning points: diabetes in older people with frailty accessed from: Key learning points: diabetes in older people with frailty | Key learning points | Guidelines in Practice 29/09/2021
- If adults with diabetes in your care have lost their appetite; lost weight; may be having difficulty eating and/or swallowing or have lost the ability to feed themselves; or have become frail or their frailty is increasing, then they are at more risk of hypoglycaemia. They should be reviewed quickly.
- Medications such as SGLT-2 inhibitors and thiazolidinediones (pioglitazone) may lead to side effects which include weight loss, dehydration, and possible toe amputations (SGLT-2 inhibitors)

Most insulin injections are prescribed in concentrations of 100units/ml, but there are insulins now available in a higher strength e.g. 200units/ml or 300units/ml. Always check the prescription and if you are unsure contact your Health Care Provider.
Risk of hypoglycaemia with insulins – doses MUST be reviewed by the health care professional.
Recommended injection sites
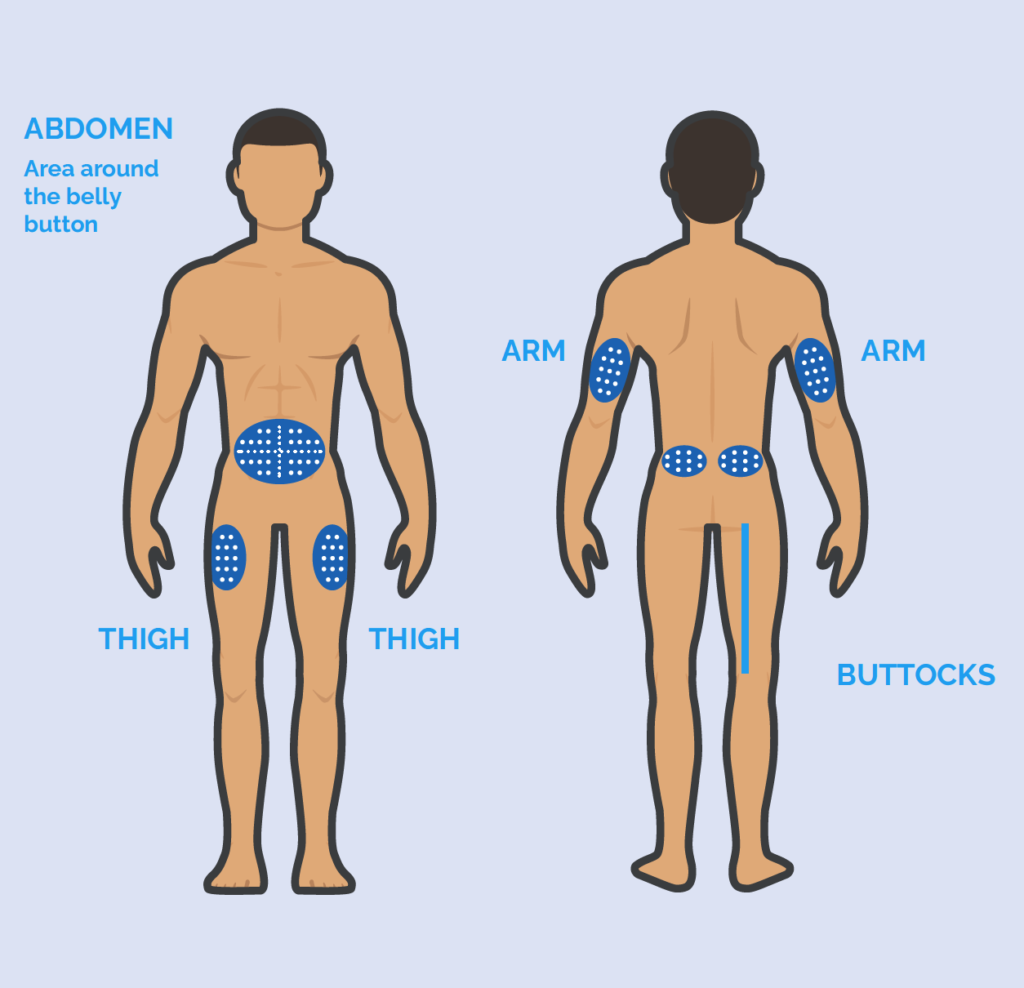
Insulin pen device(s) in-use should be stored at room temperature (avoid direct sunlight or heat e.g. radiator) – they usually expire at 28 days at this temperature EXCEPT Toujeo which expires after 6 weeks. All other insulin pen devices to be stored in the fridge (not near the freezer section) until needed.
- New needles should be used EVERY time
- Injection sites should be rotated – see chart. Using the arms is not recommended unless the person administering insulin has been trained do so due to the risk of injecting into the muscle rather than into the subcutaneous layer under the skin (access link to injection sites here: https://trenddiabetes.online/wp-content/uploads/2021/03/Guideline_ITM_2021_FINAL_v2.pdf)
- Inspect injection sites regularly for lipotrophy (fatty or hard lumps under the skin), avoid injecting into any areas that may have them because this can affect how insulin is absorbed and lead to erratic glucose readings ranging from too low or too high. https://clinicathome.swan.ac.uk/
- If administered by a Health care professional, then safety needles should always be used
- Sharps box should be available for immediate disposal of used sharps
Injection Rotation
Always follow correct injection rotation
Correct injection site rotation principles:
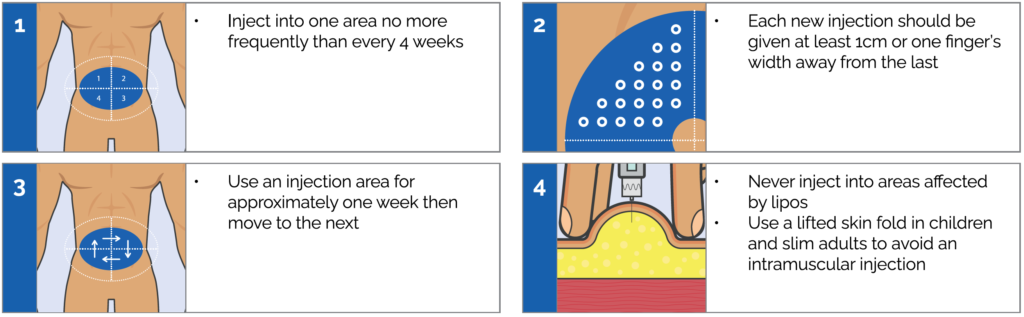
Rationale: 98% of patients with lipohypertrophy did not rotate injection sites or rotated incorrectly in a study by Smith M. Clapham L. and Strauss K, (2017) https://daneshyari.com/en/article/5587110
Images given with kind permission from Trend Diabetes For healthcare Professional: Correct Injection Technique in Diabetes Care. Best Practice Guideline (2nd ed) March 2021: https://trenddiabetes.online/wp-content/uploads/2021/03/Guideline_ITM_2021_FINAL_v2.pdf
Diabetes Treatments
Insulin in Community
Essential insulin information
Long-acting or basal
Rapid and short-acting
Intermediate
Mixed insulins
Insulin Pen Introduction
View resource that explains about lumps under the skin due to poor injection technique: What are Lipos?
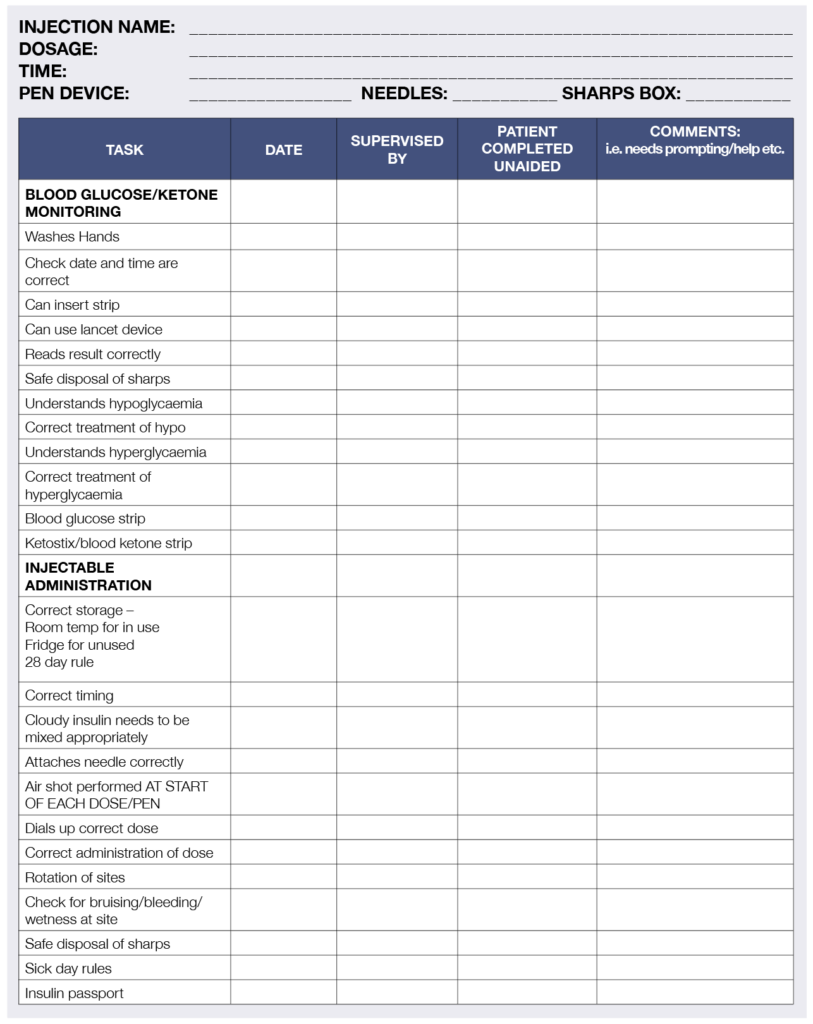
Checklist – People requiring injectable therapies
17A Medications to Manage Diabetes
17B Injectable Therapy
- 1Sinclair A (2019) Key learning points: diabetes in older people with frailty accessed from: Key learning points: diabetes in older people with frailty | Key learning points | Guidelines in Practice 29/09/2021